CBT is the abbreviation of Cognitive Behavioural Therapy, which is widely considered the McNuggets of the psychotherapeutic industry.
To start, I would say that I am personally not a hater of CBT, nor do I have any vendetta against it. As an avid philosophy reader, I find the fundamental principles of CBT to be largely intriguing. But before I expand on my view and analysis of CBT as employed in the therapeutic setting, let me briefly introduce to you what it is all about.
CBT in a Nutshell
Cognitive Behavioural Therapy (CBT) is an umbrella term for modern cognitive and behavioural therapeutic interventions. It is the first choice of treatment for many psychological disorders internationally and has become the gold standard in the field of psychotherapy. CBT is contemporarily the preferred method of treatment for depression and anxiety disorders.
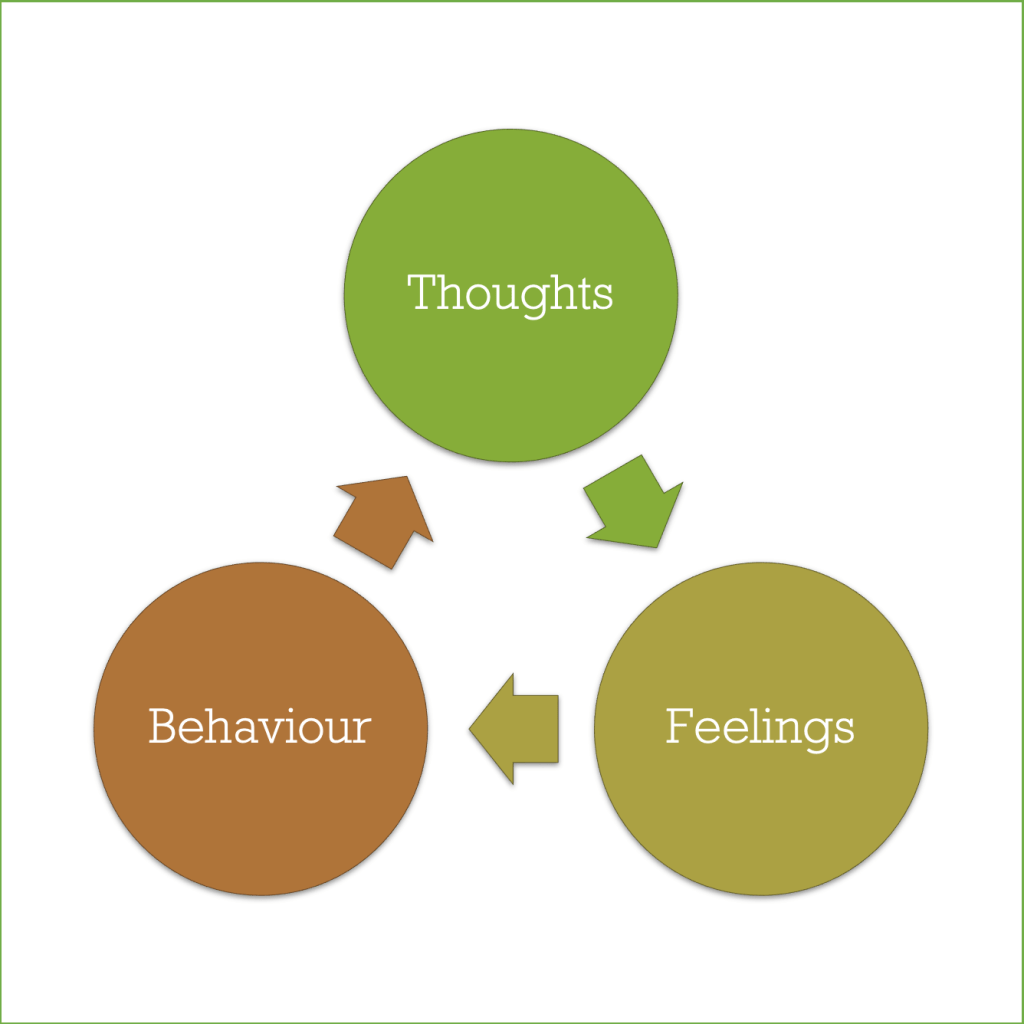
As its name suggests, CBT is principally founded upon the theory that there are intricate relationships between the workings of thoughts, feelings and behaviour in our day-to-day living experience. Thoughts are theorised to give rise to certain feelings, feelings to a more particular set of behaviour, which in turn reinforces similar thought patterns. The cognitive model of CBT hypothesises that the negative feelings someone has in the face of adversity are not caused by external events or circumstances in and for themselves, but rather by their perception of them (Beck, 1964).
‘…people’s emotions and behaviours are influenced by their perceptions of events. It is not a situation in and of itself that determines what people feel but rather the way in which they construe a situation.’
Aaron Beck
As a mode of psychological intervention, CBT practitioners are interested to look into the negative thoughts that their patients have, which they term ‘Negative Automatic Thoughts’ (NATs). They believe that NATs are rooted in dysfunctional assumptions, which are irrational and untrue. Ultimately, these dysfunctional assumptions are intimately connected to the patient’s core beliefs, which are the view of one’s self. The goal of CBT practitioners is thus to work with their patients to identify NATs, guide them to discover the underlying dysfunctional assumptions through questioning (i.e. Socratic dialectics) and offer alternative perspectives or solutions that the patients can adopt in order to rectify their maladaptive core beliefs—implicitly putting an end to the NATs and in turn makes the patients feel better in their day-to-day.

Furthermore, the three levels of cognition often correspond to what Aaron Beck (founder of Cognitive Therapy) called the cognitive triad of negative core beliefs, which are negative views about the future, the world and oneself. Below is an example of the three levels of cognitions that is intertwined with the cognitive triad, which a CBT practitioner may help their patient to uncover:
| Cognitive Level | View about… | Example |
| 1. NAT | Future | ‘Things will only get worse from here.’ |
| 2. Dysfunctional Assumption | The World | ‘Nobody likes me!’ |
| 3. Core Belief | Oneself | ‘I’m worthless.’ |
By employing multiple methods, CBT practitioners guide their patients to understand their cognition and help develop coping strategies to improve emotional regulation.
What Makes CBT So Popular?
To understand why CBT is so popular among psychological/counselling service providers and people dealing with depression and anxiety, we’ll need to first understand the scope of the issues that they are dealing with. Someone who comes to therapy and seeks help to cope with depression or anxiety is most likely struggling to well-perform their day-to-day activities (i.e. work, study, relationship-building) and possibly less satisfied with recreational activities too (i.e. leisure, hobbies). The most immediate priority of the intervention is thus centred around solving these immediate problems in the span of 30-60 minute sessions: breaking them down and setting smaller goals to develop a sense of accomplishment along the way. CBT is therefore primarily popular among patients and service providers as it’s shown to be effective within the time-limited framework.
Before CBT practitioners can work with their patients to uncover the maladaptive core beliefs that are not immediately visible, they would need their patients to help them break down and detail the activities performed in the past week and to individually rate the activities laid down on a scale of 1-10 concerning how pleasurable they find them. Subsequently, the therapist would work with the patient to set a mutually-agreed set of goals for the coming week, schedule the activities reasonably for them to be achievable and hand out ‘home works’ to sustain their practice. One key feature of the problem-solving methodology is to break tasks down into manageable steps to help overcome procrastination and anxiety-provoking situations. The first level of intervention in CBT is thus directed to change patterns of isolation and procrastination and to re-establish daily routines that provide a greater sense of enjoyment in life before the patient can deal with their dysfunctional assumptions.
For all of these reasons, why is the blog post titled the way it is? Despite its time-efficient nature and the highly structured regiments of CBT—or rather, because of it—, there is a fundamental incongruence between what a self-actualised human being could be and the solution that CBT offers. Concisely put, ‘the medium is the message’.
A Brief Philosophical Critique of CBT
My first critique of CBT is aimed at the amount of confidence and trust upon which its practitioners put into the system. In other words, I have reservations about the principles upon which CBT is founded—the Cognitive Model and the Three Levels of Cognition, among others. Furthermore, within my limited scope of study based on mock CBT sessions available on YouTube, I find it most disturbing how the sessions were led and conducted by these highly qualified CBT practitioners.
Moreover, allow me to quote a few common criticisms of CBT to keep in mind before I proceed further:
- Relative Effectiveness
- Declining Effectiveness
- High Drop-Out Rates
CBT practitioners are inclined to believe that these are due to the limited capacity and willingness of patients to change themselves. While they may be true to a certain extent, proponents of CBT do not seem reflexive enough to understand the crux of the problem regarding its approaches. Firstly, the coined term ‘Dysfunctional Assumption’ may be a clue to the core beliefs of CBT regarding human nature and intrapersonal relationships. A ‘full’ human is not reducible to a functional bio-mechanic, even if it enjoys what it does. I do not intend to rebuke a core belief of CBT based on ‘mere’ (surface-level) affective responses, but rather in view of our common appreciation and reverence for truth, right and unright. CBT can work not by virtue of its formulations, but rather by the act of the respective individual patient in taking-up responsibilities to approach their problems more authentically. While CBT practitioners can advise against the use of ‘safety behaviours’ (i.e. avoidance or escape behaviours) in more advanced sessions (Salkovskis, 1996), they cannot impart an understanding that they do not already possess—a CBT practitioner is not better than another because of their familiarity with CBT techniques, but by virtue of their experience in dealing with human contact and life’s problems more holistically.
It is also a common criticism of CBT that sessions feel ‘cold’ and that therapists are too busy engaging in dialectics to correct people’s interpretation of events. This is very much so considering that not once in the four 30-minute mock therapy sessions I watched on YouTube did I come across a ‘patient’ being asked to describe their feelings and the events leading up to it by their CBT practitioners—and this is an obvious practical example of what seems unright for me. There was a laser focus on what the patients thought about the events and they were asked to describe what these mean to them rhetorically, which seemed to me unlike a ‘guided discovery’ but more like leading questions for patients to identify with a pre-defined set of negative self-concepts (i.e. ‘I am useless’, ‘I am worthless’)—where it had been geared towards accomplishing the therapist’s agenda from the get-go.
Lastly, given how targeted the proposed solutions of CBT are, it is really not a surprise to me how only relatively effective they are on top of them being temporary—replacing dysfunctional assumptions with functional ones do not ascertain their truth, and people with integrity can only maintain functional but false assumptions for as long as they are unaware of it. It is not to say that CBT practices untruth—that would be a huge accusation and is not my point—, but rather that there is ample room for self-reflection on the part of CBT proponents and their practitioners to improve the sessions with their clients to be more holistic, engaging and fulfilling. Until then, I believe it is an extremely far-fetched statement to honour CBT as the ‘gold standard’ of psychotherapy.
Leave a comment